What is chronic pain?
Almost 7 million Canadian adults live with chronic pain. This means that 1 in 5 adults experience this chronic condition. Despite how common chronic pain is, everyone’s experience is different. This is because pain is affected by physical, psychological, and social factors. In other words, pain is affected by what is happening in our bodies, how we think and feel about it, and by the people and pets in our lives.
People learn about pain throughout their lifetime. They learn what pain means, whether to fear or accept it, and how to behave when they feel pain. Early on, pain may be helpful as a signal that something is wrong and we need to find ways to recover or heal.
But over time pain is no longer a helpful warning sign. Pain that lasts over time has negative impacts on function, relationships, and mental health. Pain is called “chronic pain” if it has lasted longer than it should based on what we know about how tissues heal.
Pain that lasts longer than 3 months is labelled “chronic”. Chronic pain may feel the same as acute pain. It can develop after an injury (e.g., car accident, surgery, fall), disease (e.g., arthritis), or for no apparent reason. Chronic pain can last even after an injury or disease has healed because of changes in how the nervous system processes information.
Does my pain have to be constant to be chronic?
Chronic pain isn’t constant. You don’t have to be living with pain all day, every day to have chronic pain. Your pain may come and go throughout the day. Or you might have pain for a few days, weeks, or months at a time. Chronic pain fluctuates and can change in severity, becoming better or worse during the day, and over time. The effects and symptoms of chronic pain are different for everyone.
What are the different types of pain?
There are three main types of pain: nociceptive pain, neuropathic pain, and nociplastic pain.
Nociceptive pain
Nociceptive pain is developed when special nerves are activated that report information about potential or actual harm to our tissues (e.g. bones, muscles, ligaments, organs, skin). These nerves are active when we come into contact with threats. Threats can be things like too much pressure on or stretch of our tissues, limited blood flow, objects or environments that are too hot or cold, inflammation in the tissues, or a chemical burn on the skin. This type of pain usually gets stronger when the threat or damage is greater. It can get better when the threat or damage is gone.
Neuropathic pain
Neuropathic pain comes from damage to a part of the nervous system, such as a nerve, the spinal cord, or brain. This type of pain will be different depending on what part of the nervous system is affected and how it is affected. This pain often feels like an electric shock, prickling, or sharp, stabbing pain. Numbness can also happen. Things that normally don’t cause pain can trigger this type of pain. For example, a gentle touch on the skin can feel overly sensitive or like a sharp pain.
Nociplastic pain
Nociplastic pain is sometimes called “pain amplification syndrome” or “central sensitization syndrome”. This type of pain develops when the central nervous system, meaning the spinal cord and brain, changes how information is processed. With this type of pain, pain can be felt even though there may be nothing or very little wrong with body tissues. Someone may or may not have had an injury in the past that started the pain. But now the pain continues and may spread to other areas.
Despite the different types of pain, chronic pain can show itself in many ways.
What are the signs and symptoms of chronic pain? Does chronic pain show itself in different ways?
Chronic pain can feel like:
- Sharpness
- Aching
- Dullness
- Pins and needles
- Burning
- Shooting
- Throbbing
- Numbness
- Tenderness
- Tingling
- Unbearable
Chronic pain may make you feel:
- Tired / Fatigued
- Irritable
- Nauseous
- Angry
- Frustrated
- Depressed
- Anxious
- Hopeless
- Mentally or physically exhausted
How your pain feels and how it affects you may be different from what other people describe. This is because your pain is unique because you are too.
What causes or triggers chronic pain?
Chronic pain can be caused for a variety of reasons: ongoing problems related to an injury (e.g., an amputation), chronic illness or diseases, inflammation, damaged nerves, or changes in how the brain processes information. Sometimes, chronic pain begins for no specific reason (e.g., migraines). Chronic pain can also be affected by the environment we live in. Environmental and situational triggers can include things like foods, body positions, activities, weather changes, a light touch on or close to the affected area, physical activity, hot or cold weather.
How is chronic pain treated?
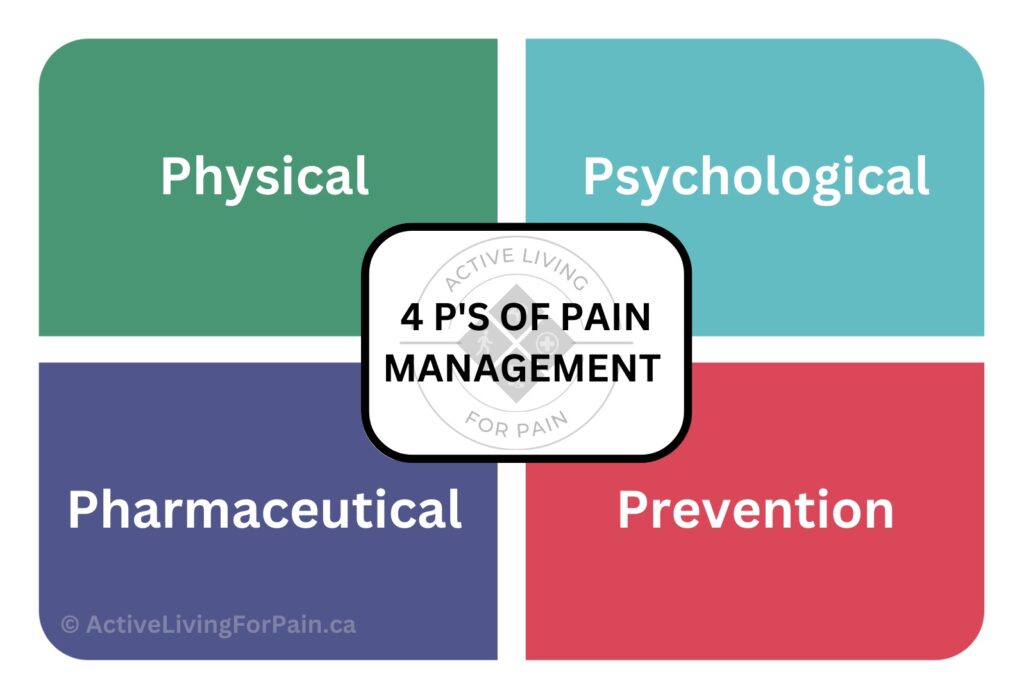
There are lots of ways to treat chronic pain. Treatment can depend on what kind of pain you have, the way your chronic pain developed, your age, and health status. There are four main categories of treatment strategies for pain management. These categories are known as the 4 P’s of Pain Management.
The 4 P’s include prevention, psychological, physical, and pharmacological strategies that can be used to help improve pain. The best results happen when you use a combination of different strategies. Click here to learn more about the 4 P’s of pain management.
What treatments are the right ones to manage your chronic pain?
Prescribing opioid medications is no longer the first step that is recommended for treating chronic pain. There are several other strategies that are recommended and effective for managing pain. Please explore the links below for more information about chronic pain and management strategies.
- Physical activity
- Self-management tools
- The 4 P’s of Pain Management
- Saskatchewan Health Authority Chronic Pain Resources